October 2021
In this VETgirl online veterinary continuing education blog, Dr. Hillary Israeli, VMD, BFD, PennVet 2000 shares how to MacGyver your way in veterinary life. Because sometimes you need to think creatively in desperate situations, and if there’s one thing I know about veterinary professionals, it’s their ability to think creatively, think under pressure and MacGyver the crap out of #vetmed. For you youth who don’t know what “MacGyver” is, it’s the amazing TV series with Richard Dean Anderson in the 80’s, yo. Huge kudos to Dr. Israeli, who I had the honor of knowing while at PennVet, for saving this cat. One life down, 8 to go.
Sugar rush in the crashing diabetic veterinary patient
By Dr. Hillary Israeli, VMD, BFD, PennVet 2000
I am still feeling the adrenaline rush from this one.
I saw a cat (12 year-old DSH, MN) on Monday whose concerned owners had noticed he was drinking and peeing more than normal for several weeks. He weighed 22.2 lbs, up from 20 about 8 mos prior. His people hadn’t noticed any additional problems – he ate well, used his litter box, and seemed to be his normal self. They used to feed him Hill’s Metabolic diet, but due to supply issues last year they had switched to Hill’s adult/senior light cat food. I suppose this might be partly responsible for what happened next.
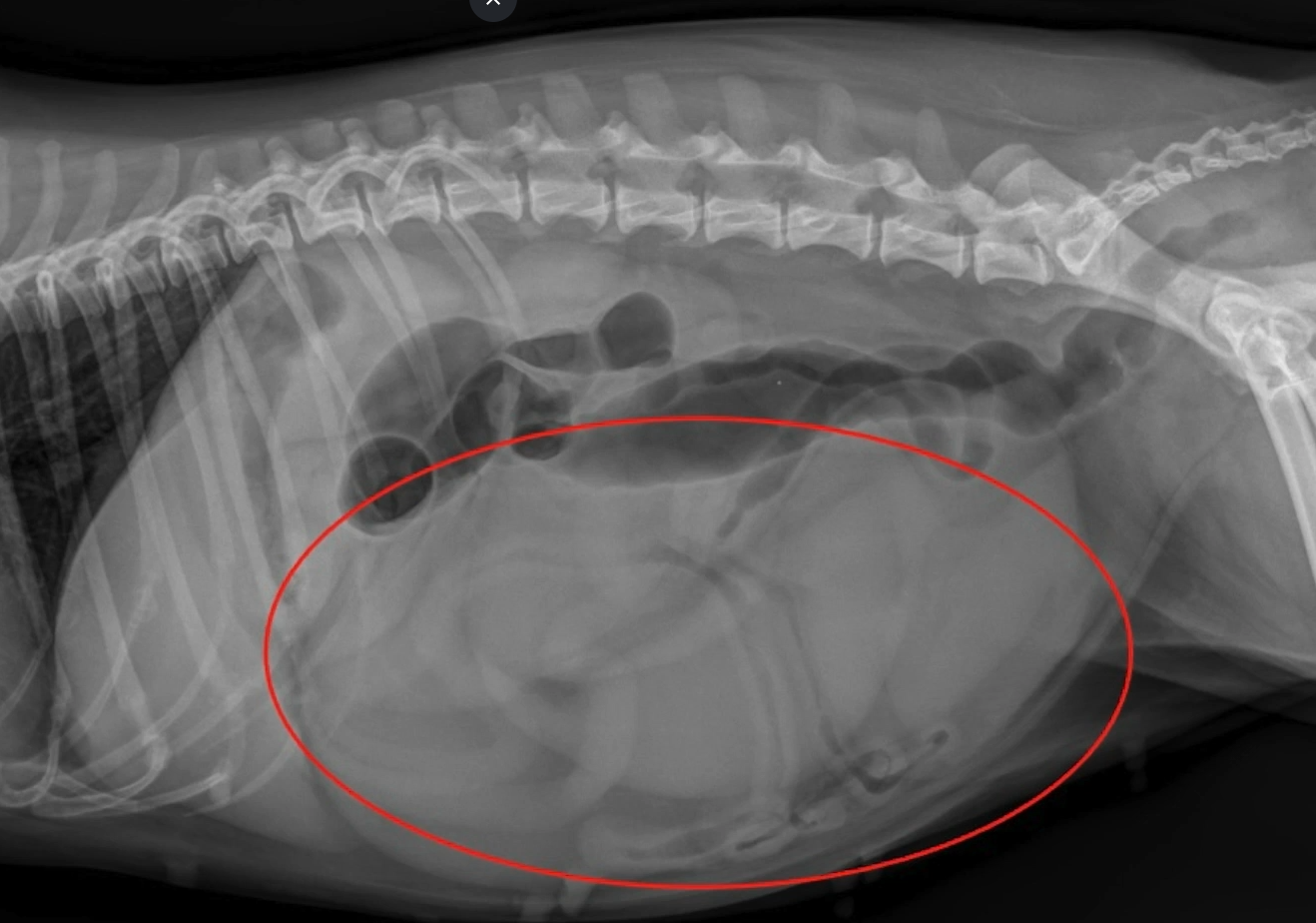
On physical exam, Tidbit was obese and unkempt, but otherwise normal. Labs revealed uncomplicated diabetes mellitus: blood glucose 461 mg/dl, urine glucose 3+ but nothing else significant. I went over all the usual stuff with them carefully when I called them with the results on Tuesday: my plan was 2 u Lantus BID – feed to ensure eating first (not likely to be a problem with this guy!) – and schedule a tech visit with the female owner, to go over the insulin administration. I wrote prescriptions for everything – insulin type and dose, syringe needle length, volume, units of measurement – everything in writing to avoid problems or confusion because, frankly, I am sick of pharmacy staff convincing my clients they don’t mean what I told them to say, or that they must be confused, or that somehow they can save hundreds of dollars by switching to a different product, or whatever. So this very nice, concerned couple came over to pick up the packet of information and prescriptions, and as they were heading out, the man said that by the way, they didn’t need the tech visit – they had had a pet with diabetes before, and had used insulin shots for ten years, and were sure they felt very comfortable with the process. This seemed reasonable to me – the facts checked out – I didn’t object. LESSON LEARNED!
You may be guessing where this is going….but probably not the entire thing.
The owner of the hospital where I work, who is a personal friend of these cat owners, phoned me at 6:45 AM Wednesday and blurted out “SO sorry to bother you Hillary, but JD found Tidbit seizing in the bathroom around half an hour ago. They tried putting maple syrup in his mouth but it isn’t helping. He gave the first dose of insulin – he said he gave 2 units – last night, and says he ate his whole dinner and seemed fine when they went to bed.” I said “He needs to go to the ER. I’m at least half an hour away and this is an actual emergency.” She said ok. Expecting that Tidbit was en route to one of the many local vet ERs we are blessed to have around here, I finished breakfast, got in the car, and went to run an errand involving some sports equipment for my daughter, who is captain of her high school tennis team. At about 7:20 AM, I called my boss from the parking lot of the sports equipment shop, and asked for a status report on the cat – had he been admitted somewhere? She said “well, they’re coming to the clinic now,” I said “what? OUR clinic?” she said “yeah, they didn’t want to go to the ER, they want us to look at him…” So, I said “well thank dog I was running an errand near work b/c I can be there in five minutes see you soon.” I hauled ass over there, cat arrived 3 minutes later, and YOU WON’T BELIEVE WHAT HAPPENED NEXT.
Ha ha.
Picture this: it’s 7:30 am, and I have just examined the cat. I have determined he’s shocky, peripherally vasoconstricted with cold extremities and purplish feet, bradycardic w/HR around 75, non-responsive to most stimuli including a tap on the cornea, he’s twitching, his head and neck are sticky from maple syrup and drool, and a quick needle stick tells me he is hypoglycemic below the range detectable by my glucometer. The owner was telling me he thinks maybe the cat’s feet are cold from the ice packs he put on the cat to him when he found him, either before or after he gave him the maple syrup on his gums. I tried not to think about that while focusing on my next step.
I managed somehow to get IV access and a working catheter, but I could not find any damn dextrose to save my life. I ran all over the clinic and called everyone I could think of. At first, no one else was even there because we don’t open til 9 and my boss had LEFT to go pick up one of our techs so she could come in early to help. During the chaos, a few staff started to trickle in and I cannot thank them enough for their level-headed assistance! Props to Bernie W for finally securing the IV cath from hell, by the way.
I set the clients to the task of calling all local pharmacies etc to see if they could find any injectable dextrose but this cat could not wait. I mean, I knew he would not make it to the ER at this point. So – grabbed sugar packets from the break room, poured them into a (clean) Starbucks cup, added water to make a sugar solution, and boiled it in the microwave for a minute.
Don’t forget to use a clean Starbucks cup. Then I added more cold sterile saline to bring the temperature down to injectable level and then I just kept giving the cat boluses of that.

Don’t forget to microwave your water to boil it and “sterilize” your homemade dextrose solution… Photo courtesy Dr. Hillary Israeli

Might be the cleanest veterinary microwave this VETgirl has ever seen, so it looks sterile. Photo courtesy of Dr. Hillary Israeli
Eventually the cat started to get more responsive. He was pink. His feet were warm. He vocalized a bit. He no longer tolerated a finger touching his eyeball. His HR came up to a more normal rate. Repeat BG 280 mg/dl. OMG. That worked??!!
I got slightly calmer until I saw that those leg twitches were turning into leg excursions and cat was going into a full blown tonic-clonic seizure. It was at that point that the cavalry arrived in the form of my colleague Dr. H, who had apparently walked in, seen what was going on, and was already drawing up midazolam when I heard someone walking down the hall and yelled out “would someone please grab me the controlled drugs he’s gonna seize again” and I think it was in my hand before I finished even saying it so I gave that and he relaxed.
At some point after that, the cat started to twitch again, and then paddle, and then started to have abdominal contractions and look like he was ready to vomit, so I gave one more dose of midazolam, and some Cerenia too, which helped.
We got a vial of 50% dextrose for IV injection from the vet hospital down the road once they opened, and the intrepid Dr. H stepped in again to do some fancy math while I was monitoring the patient. We hung the bag of carefully concocted 2.5% dextrose in saline, and sent the cat out the door to Heroes Unlimited (aka the local vet ER) at around 9:30 AM with a BG of 190, enough neurons to lie in a sternal position and to vocalize and to blink and gag, and a chance at life, I guess.
I went into my office to call the ER about this situation, and found that my colleague had helpfully put the total midazolam we used that day on a sticky note on my desk near where we store the drug logs before she headed into surgery on her own patients. Thank goodness for colleagues who care! Note to self: bring donuts for everyone next week!
Luckily for me – when I called to give a heads up about my train wreck referral, instead of asking me what the hell my problem was and urging the client to file a board complaint, the receiving veterinarian on the other end just said something like “Wow. OK. Wow.” Clearly, she understood where I was coming from. That was a relief.
But seriously, I may never be the same. I don’t do ER. I don’t do complex fluid math under stress. I dislike using things “to effect” on a good day. I like rules and algorithms! Also, gaining IV access in a shocky bradycardic seizing cat with cold peripheral limbs is no mean feat.
HOW DID THIS HAPPEN, you may wonder. I mean, ok, so it’s probably obvious but for the historical record – the owner showed me his insulin syringes and pointed to the line he filled it up to, and as you probably suspected, he had given the cat 20 units, not 2, because he thought it said “2.0” not 20. Could this have been prevented by a tech visit as originally planned? Probably. But that’s water under the bridge – this owner was shocked, horrified, embarrassed, and ashamed, and there seemed to be no point in pressing the matter. I told him that everyone makes mistakes, some mistakes have more devastating effects than others, and that we should focus on trying to prevent future mistakes, not dwelling on old ones. I mean, in the moment, what else is there to say, really?
You might also ask how on Earth we had no dextrose in the clinic. I certainly asked! But apparently, although we had in fact placed an order for some — it hadn’t come in. It had slipped through the cracks when we ran out, because no one needed it for a while, and we ran out before our next scheduled inventory/order reconciliation. Anyway, I didn’t have time to waste thinking about that at the time. I had more pressing problems, like the fact that my 9 AM new client, with two new patient dogs, had been sitting patiently across the hall for something like 45 minutes or an hour already. So, I just took a deep breath and walked into the room.
THAT is when I learned that this new client, although no longer in clinical practice, was in fact formerly an ER vet at the exact hospital I had just gotten off the phone with. She asked if I were ok, and suggested I go take a pee break and get some water before seeing her dogs. I almost cried then! How lucky was I to be met after such chaos by such an understanding person?
And I just now (Friday morning) received the discharge report from the ER: the cat was discharged – mentally dull, and probably blind, but ambulatory and eating and possibly continuing to improve. I cannot believe this even happened.
How was your week?
Dr. Hillary Israeli, VMD, BFD, PennVet 2000
——
The geeky details:
One Domino sugar packet in the USA contains 3.5 g sugar.

D50W (50% dextrose in water for injection) is roughly 50 g sugar in 100 ml H2O, or 25 g sugar in 50 ml, or 12.5 g in 25 ml.
That’s ROUGHLY 14 sugar packets to make 100 ml 50% solution, or 7 sugar packets to make 50 ml of a 50% solution, or 4 packets to make 25 ml solution.
WHAT I DID: I took 4 packets of sugar and enough water to cover it up in a tall Starbucks cup, and microwaved it for a minute. Then I added cold sterile saline to approximately 25 ml volume, which I happen to know from years of experience in the kitchen is the level of the top of the small square marked “drink” at the bottom of the column of squares on the side of a Tall Starbucks paper to go cup. Still seemed kinda hot when I splashed some on my wrist so I added more saline and probably ended up with about a 20-30% solution based on my eyeballing it. Then I just kept giving that until the cat seemed to be improving and had a BG >200. Then, we hooked him up to a bag of 2.5% dextrose in normal saline that my colleague put together using a bottle of borrowed D50W we got from a neighboring clinic which had finally opened.
Don’t try this at home, folks. Emergency situation, however? Saved this cat.
VETgirl explains how to make that solution here: https://vetgirlontherun.com/dos-and-donts-of-dextrose-vetgirl-veterinary-continuing-education-blog/
P.S. Happy Halloween! Don’t let your patients get into too much sugar (e.g., theobromine/chocolate).
Only VETgirl members can leave comments. Sign In or Join VETgirl now!













YOU GET THE “WHAT A WOMAN” AWARD
BFD vet for sure! Nice work!!
What a very entertaining read! This story had me gasping, jaw dropping, smiling, and laughing…and maybe even tearing up a little. 🙂 Well done!
I am in awe and feeling empowered to meet this moment in another dimension. More than Kudos is due to you!!
Amazing story! Thanks for sharing!